There is plenty of research available pointing towards the positive influence a healthy gut microbiome can have on your overall health. But how do you know what’s really going on inside you?
While symptoms such as bloating, gas, indigestion, and even some skin disorders may be the result of an imbalanced gut, the only way to properly gauge the diversity of your gut, is through microbiome testing.
So, join us on a journey of discovery as we find out what a gut microbiome test is and how human milk oligosaccharides can help boost the good bacteria in your own gut microbiome.
What is the gut microbiome?
The gut microbiome is the term given to the bacteria and their genes residing in your gut. You may also have heard the term ‘gut microbiota.’ Although these terms are used interchangeably, there is a slight difference in that the microbiota is the collective term for your gut bacteria but not including their genes.
What is gut microbiome testing?
One way to literally ‘see’ how your gut microbiome looks is using a gut microbiome test. Microbiome tests use a sample of your feces to analyze the microbes and any potential imbalances within your gastrointestinal system.
How does a gut microbiome test work?
When you sign up for a gut microbiome test, you’ll be required to provide a stool sample. Depending on the company you choose, this could be just a small amount or an entire sample.
Traditionally, a stool sample would be sent away for laboratory analysis to look for bacteria that cause infections. However, advancements in testing mean that companies now analyze the composition of your gut microbiome using a stool sample.
The analysis they conduct can help to show how many different bacteria are present through DNA sequencing. Some tests will also measure some of the biomarkers associated with gut health. For example, they may measure the amount of inflammation present.
What can gut microbiome tests tell you?
At-home microbiome tests can be considered a first step in understanding more about your gut. However, this should be for your own information rather than for clinical or diagnostic purposes. If you have any gastrointestinal symptoms, you should consult your doctor for advice.
A gut microbiome test may tell you about the different types of bacteria residing in your gut as well as the overall composition and diversity. So, you may be able to identify certain species that are abundant or those that might need to be boosted.
Can you ‘boost’ the composition of your gut microbiome at home?
Your gut microbiota is a valuable army of microbes that, amongst many other things, help to digest the dietary fiber your body is ill-equipped to do. By breaking down the fiber and transforming it into useful metabolites your body can use, the abundance and activity of certain species of bacteria will increase.
Here are some of the ways you can help to boost your gut microbiome.
- Eat a range of foods
- Make sure your diet contains plenty of plant foods
A study by Klinder et al. (2016) found that increasing fruit and vegetable intake, as well as flavonoids, had an inhibitory effect on pathogenic clostridia species. While other research shows that eating a diet rich in wholegrain foods can promote the growth of health-promoting species such as Bifidobacteria and Lactobacilli. Interestingly, a British study conducted in 2008 found that daily consumption of a whole grain, wheat-based breakfast cereal had a significant prebiotic effect on the composition of the human gut microbiome.
Get Some Prebiotic Fiber into Your Diet
PureHMO® human milk oligosaccharide from Layer Origin Nutrition is an example of a powerful prebiotic. By supplementing your diet with PureHMO® you could reap numerous benefits, including:
- supporting the health of your gut microbiome
- providing nourishment for important health-promoting bacteria
- supporting your cognitive function
- experiencing relief from IBS symptoms
In breastfed babies, HMOs are a vital food source for the bacteria in the infant gut, helping to shape the developing microbiome. However, emerging science suggests that HMOs are also important for modulating the immune system and are an important factor in preventing the adhesion of pathogens. However, PureHMO® is NOT derived from human breast milk. It is produced by precise fermentation of lactose (cow’s milk).
The PureHMO® range features a mix of high purity HMOs, including 2’-Fucosyllactose (2’-FL) and Lacto-n-Neotetraose (LNnt). Research conducted in mice shows that 2’-FL supplementation can reduce intestinal inflammation and decreases the severity of colitis (a chronic condition where the colon and rectum are inflamed).
Further studies show that 2’ FL is able to boost Bifidobacteria counts as well as increase the production of short-chain fatty acids (SCFAs), including butyrate – a potent health promoter[xii].
So, supplementing your diet with HMOs can have some powerful health benefits, including promoting the diversity of your gut microbiome, increasing the activity of butyrate-producers, and relieving gastrointestinal symptoms.
What effect does PureHMO prebiotic have on the human gut microbiome?
It’s great reading the scientific literature, but what about the benefits of Layer Origin’s PureHMO®? How can we ‘see’ them for ourselves? A gut microbiome test allows us to peek inside our guts and see what’s really going on. That’s exactly what we did with one of our consumers – and the results speak for themselves.
Before taking any HMOs, the consumer had undetectable levels of Bifidobacteria in their gut. However, after supplementing their diet with PureHMO® and completing a further gut microbiome test, the consumer’s Bifidobacteria abundance increased by a whopping 2582% (yes, you did read that right) in just 23 days.
Bifidobacteria are a probiotic species that are natural residents of the human gut. They are often among the first colonizers of the gut when you are born and are renowned for their adaptive abilities and beneficial health properties. They are also known for their cross-feeding abilities – the metabolites they produce help to nourish bacteria that produce butyrate.
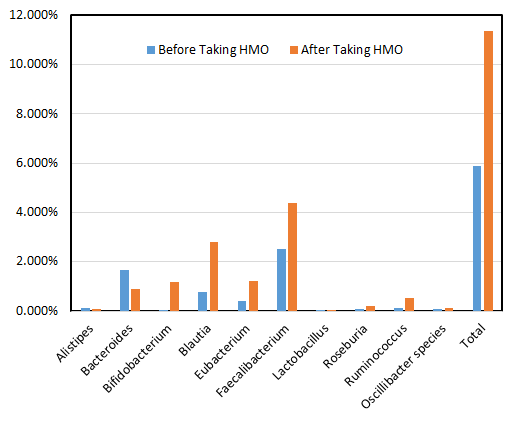
Figure 1 shows the increase of good bacteria before and after taking PureHMO® 2'FL (2 scoops/day) for 23 days. The detailed data was also showing below:

Figure 1 demonstrates the increase in several healthy gut bacteria species, including:
- Bifidobacteria
- Blautia
- Eubacteria
- Faecalibacterium
- Roseburia
- Ruminococcus
- Oscillibacter spp.
- Total good bacteria
The results of the test also show a 173% increase in Faecalibacterium, specifically F. prausnitzii. The study by Ryan et al. (2021) also noted an increase in the abundance of F. prausnitzii in the stool samples of the study participants. Interestingly, specific strains of Bifidobacterium longum have been shown to increase their production of the SCFA, acetate, when cultured in 2’-FL. This is interesting because acetate helps to feed butyrate producers like F. prausnitzii, which have been linked to numerous health benefits and could be considered a therapeutic approach to managing both irritable bowel syndrome (IBS) and irritable bowel disease (IBD).
Conclusion
Although home gut tests shouldn’t be used for diagnostic purposes, they can offer insights into the composition and diversity of your gut microbiome. They can also demonstrate how well your supplements are working and if they are doing what they say they do. The results from our consumer showed that after just 23 days of using the PureHMO® supplement, the abundance of total good gut bacteria increased from 5.782% to 11.214%.
If you want to ensure your gut microbiome is abundant with good bacteria species, you can learn more about PureHMO® here.
Written By: Leanne Edermaniger, a science writer who enjoys writing about all things related to the gut microbiome.
References:
[i] Brody, H., 2020. The gut microbiome. [online] Nature.com. Available at: <https://www.nature.com/articles/d41586-020-00194-2> [Accessed 11 October 2022].
[ii] Carding S, Verbeke K, Vipond DT, Corfe BM, Owen LJ. Dysbiosis of the gut microbiota in disease. Microb Ecol Health Dis. 2015 Feb 2;26:26191. doi: 10.3402/mehd.v26.26191. PMID: 25651997; PMCID: PMC4315779.
[iii] Staley C, Kaiser T, Khoruts A. Clinician Guide to Microbiome Testing. Dig Dis Sci. 2018 Dec;63(12):3167-3177. doi: 10.1007/s10620-018-5299-6. Epub 2018 Sep 28. PMID: 30267172.
[iv] David LA, Maurice CF, Carmody RN, Gootenberg DB, Button JE, Wolfe BE, Ling AV, Devlin AS, Varma Y, Fischbach MA, Biddinger SB, Dutton RJ, Turnbaugh PJ. Diet rapidly and reproducibly alters the human gut microbiome. Nature. 2014 Jan 23;505(7484):559-63. doi: 10.1038/nature12820. Epub 2013 Dec 11. PMID: 24336217; PMCID: PMC3957428.
[v] Sonnenburg ED, Smits SA, Tikhonov M, Higginbottom SK, Wingreen NS, Sonnenburg JL. Diet-induced extinctions in the gut microbiota compound over generations. Nature. 2016 Jan 14;529(7585):212-5. doi: 10.1038/nature16504. PMID: 26762459; PMCID: PMC4850918.
[vi] Klinder A, Shen Q, Heppel S, Lovegrove JA, Rowland I, Tuohy KM. Impact of increasing fruit and vegetables and flavonoid intake on the human gut microbiota. Food Funct. 2016 Apr;7(4):1788-96. doi: 10.1039/c5fo01096a. PMID: 26757793.
[vii] Tangestani, H., Emamat, H., Ghalandari, H. and Shab-Bidar, S., 2020. Whole Grains, Dietary Fibers and the Human Gut Microbiota: A Systematic Review of Existing Literature. Recent Patents on Food, Nutrition & Agriculture, 11(3), pp.235-248.
[viii] Costabile, A., Klinder, A., Fava, F., Napolitano, A., Fogliano, V., Leonard, C., Gibson, G. and Tuohy, K., 2007. Whole-grain wheat breakfast cereal has a prebiotic effect on the human gut microbiota: a double-blind, placebo-controlled, crossover study. British Journal of Nutrition, 99(1), pp.110-120.
[ix] Slavin, J., 2013. Fiber and Prebiotics: Mechanisms and Health Benefits. Nutrients, 5(4), pp.1417-1435.
[x] Bode, L., 2012. Human milk oligosaccharides: Every baby needs a sugar mama. Glycobiology, 22(9), pp.1147-1162.
[xi] Grabinger, T., Glaus Garzon, J., Hausmann, M., Geirnaert, A., Lacroix, C. and Hennet, T., 2019. Alleviation of Intestinal Inflammation by Oral Supplementation With 2-Fucosyllactose in Mice. Frontiers in Microbiology, 10.
[xii] Ryan JJ, Monteagudo-Mera A, Contractor N, Gibson GR. Impact of 2'-Fucosyllactose on Gut Microbiota Composition in Adults with Chronic Gastrointestinal Conditions: Batch Culture Fermentation Model and Pilot Clinical Trial Findings. Nutrients. 2021 Mar 14;13(3):938. doi: 10.3390/nu13030938. PMID: 33799455; PMCID: PMC7998190.
[xiii] O'Callaghan A, van Sinderen D. Bifidobacteria and Their Role as Members of the Human Gut Microbiota. Front Microbiol. 2016 Jun 15;7:925. doi: 10.3389/fmicb.2016.00925. PMID: 27379055; PMCID: PMC4908950.
[xiv] Belenguer A, Duncan SH, Calder AG, Holtrop G, Louis P, Lobley GE, Flint HJ. Two routes of metabolic cross-feeding between Bifidobacterium adolescentis and butyrate-producing anaerobes from the human gut. Appl Environ Microbiol. 2006 May;72(5):3593-9. doi: 10.1128/AEM.72.5.3593-3599.2006. PMID: 16672507; PMCID: PMC1472403.








